|
Dead space fraction calculation using the estimate from physiological variables and the ventilatory ratio at day 2 showed independent association with mortality at 30 days (odds ratio 1.28, p < 0.03 and 1.20, p < 0.03, respectively) whereas, the Harris–Benedict and Penn State estimations were not associated with mortality. Estimated dead space fraction and the ventilatory ratio at days 1 and 2 were significantly higher among non-survivors ( p < 0.01). Individual patient data from 940 ARDS patients were analyzed. The present study is a post hoc analysis of a prospective observational cohort study of ICUs of two tertiary care hospitals in the Netherlands. This study aimed to compare various methods for dead space estimation and the ventilatory ratio in patients with acute respiratory distress syndrome (ARDS) and to determine their independent values for predicting death at day 30. This study provides pathophysiologic justification for the use of established ARDS therapies in COVID-19, including low tidal volume and early prone ventilation.Indirect indices for measuring impaired ventilation, such as the estimated dead space fraction and the ventilatory ratio, have been shown to be independently associated with an increased risk of mortality. These findings differ from those in the early series that described near-normal respiratory system compliance and lack of recruitability in patients with COVID-19 respiratory failure. Successfully extubated - 41 patients (62%).Median duration of mechanical ventilation - 16 days.While supine 72 hours after initial prone positioning - 233 and 42Īs of April 28, 2020, after a median follow-up of 34 days (range, 30-49):.After returning to supine position - 217 and 35.In the supine position immediately prior to prone positioning - median PaO2:FiO2 was 150 and median compliance was 33 mL per cm H2O.Thirty-one patients underwent prone ventilation for a median of two sessions (range, 1–3), with a median of 18 hours per session: Similar parameters have previously been observed in large cohorts of ARDS patients. Estimated physiologic dead space ratio - 0.45.Static compliance of the respiratory system - 35 mL per cm H2O.On ICU admission, 56 patients (85%) met Berlin criteria for ARDS, mostly mild to moderate. Positive end-expiratory pressure (PEEP) was titrated per institutional protocols, which included use of the lower PEEP/higher FiO2 ARDS Network table, titration by best tidal compliance and esophageal manometry. Early consideration of prone ventilation for partial pressure of arterial oxygen to fraction of inspired oxygen ratio (PaO2:FiO2) 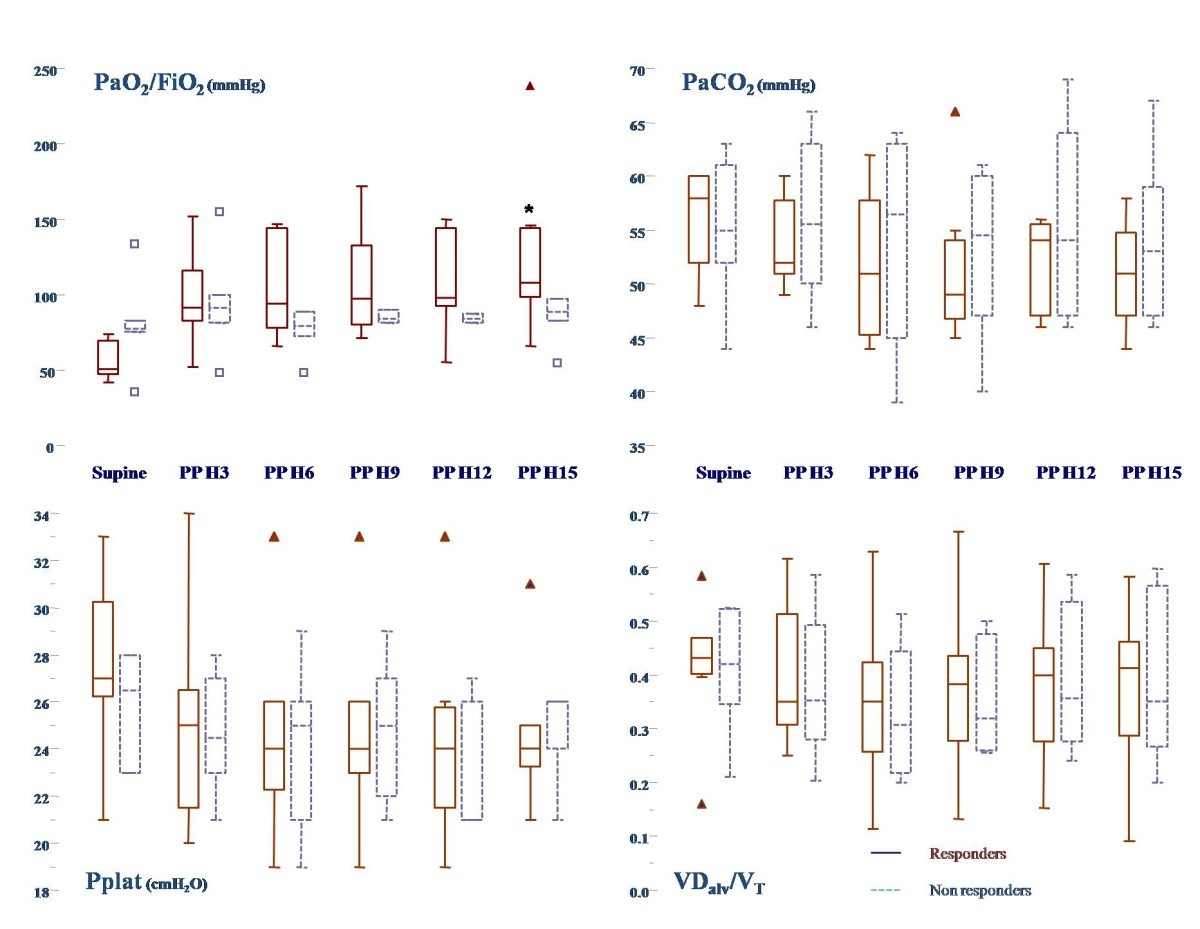
Ventilation with tidal volumes Treatment guidelines at both hospitals recommended: Management was at the discretion of the treating physician. The case series includes all 66 adult inpatients with respiratory failure related to COVID-19 who were intubated and admitted to an ICU at Mass General or Beth Israel Deaconess Medical Center between March 11, 2020, and March 30, 2020. Ziehr, MD, of the Division of Pulmonary and Critical Care Medicine at Massachusetts General Hospital, and colleagues refute this notion in a report on 66 patients published in The American Journal of Respiratory and Critical Care Medicine. Physician-scientists Corey Hardin, MD, PhD, and Jehan Alladina, MD, and clinical fellow David R. 
Error: Please enter a valid email address.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
